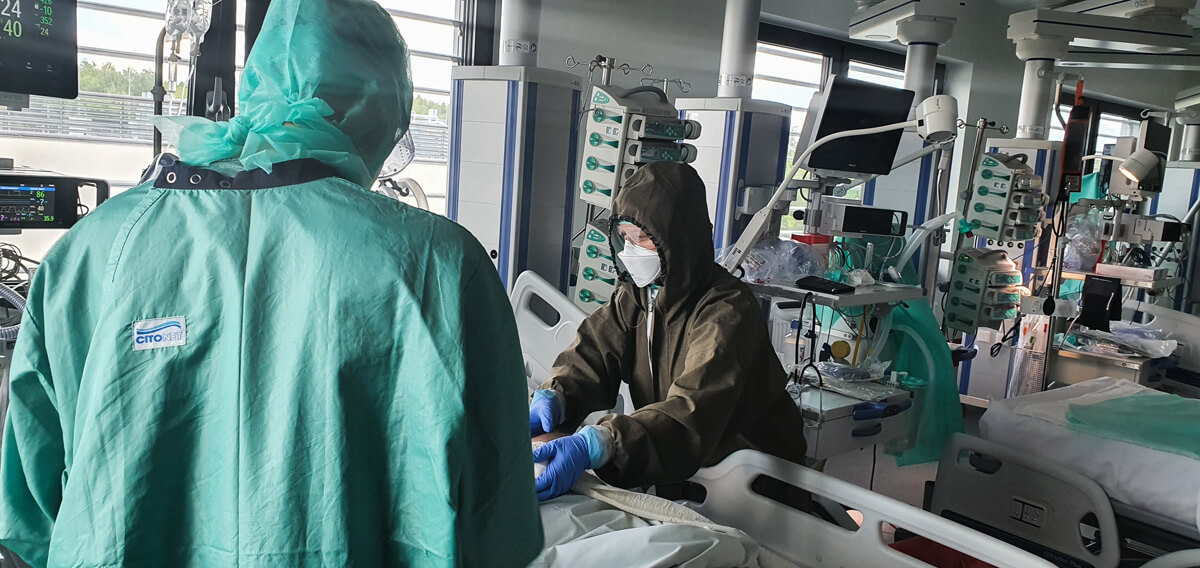
Physiotherapists from the Intensive Care Unit at the University Hospital in Cracow work in a team which treats and mobilizes patients in the most critical conditions. We work in a very big department with 65 beds for intensive care and full range of techniques applied in treating serious infections of the respiratory system – from high-flow nasal cannula (HFNC), through non-invasive ventilation (mask- and helmet-based), advanced conventional ventilation, to ECMO. It is not an easy job but after a few years of experience we were convinced that it wasn’t so mysterious to us anymore. It also stopped being such a psychological burden, when compared to the beginning of our careers.
An unknown intruder
Or at least that’s what it seemed like until the outbreak of COVID-19. Although we’ve already had some experience with patients infected with SARS or AH1N1, this virus has surprised us all. It was something completely new and unidentified. Just like the majority of our fellow medics, we were really confused and worried. At first we didn’t have any detailed information about the virus itself. We had to rely on our intuition and previous experience. Thankfully, there has been some progress in research and more secrets about this intruder are being revealed.
We have prepared our own internal model of working with patients infected with SARS-CoV-2 patients, based on the guidelines issued by the Polish Chamber of Physiotherapists. We thoroughly discussed every case with an attending physician. The disease often progressed very rapidly – one day we would talk with a patient and on the next day he would already be intubated. We therefore had to make quick decisions regarding corrections in our therapy plans. The therapy had to be adjusted to a patient’s current condition. Apart from clinical work, we also organized numerous teleconferences, discussed latest research with our colleagues, exchanged experiences and information about patients who returned to the ICU several times. Below we present a brief summary of our experiences from working in the COVID-19 zone for the last couple of months.
The character of work in the area of epidemiological danger
The first entry to the COVID zone is accompanied by fear, uncertainty and some kind of thrill. Many layers of protective clothes make it difficult to move, communicate or breathe. The order of both putting on the elements of protective equipment (uniforms, masks, visars, goggles) but most importantly of taking them off, plays a crucial role, as the risk of infection is exceptionally high in those moments, as the experience of Italian medics has shown. So this part of our work is the most disturbing. Protective uniform allowed us to work for the maximum time of three hours. After that, we were obliged to take a shower twice and undergo disinfection.
Fortunately, there was no shortage of personal protective equipment at the University Hospital. It really improved our psychological comfort. Since we all looked the same, we couldn’t really recognize each other. In some moments it even turned out to be quite funny and brought smiles on our colleagues’ faces covered with masks. No one paid attention to how they looked – the only thing that mattered was a fight for breath – our own and our patients’.
Each of us needed at least 2-3 hours of sleep after coming home from work. That is quite a good indicator of how stressful was every entrance to the “infected zone”.
The character of physiotherapy for patients infected with coronavirus
Physiotherapists who entered the areas of epidemiological danger on different wards of the University Hospital have worked out specific systems applicable to each ward. The methods of rehabilitating COVID-19 patients who stayed in the Intensive Care Unit differ only slightly from the techniques of daily rehabilitation implemented on our ward. Every patient should be approached individually and therapy plans should be dynamically adjusted to a patient’s changing condition. Constant consultations with other members of the medical staff are necessary. We have observed that patients infected with SARS-CoV-2 virus characterize with very low tolerance of physical effort. First attempts at verticalization must be conducted under careful eye of a physiotherapist and attending physician, with constant observation of vital parameters.
Frequently applied techniques
- Exercises for tromboprophylaxis – SARS-CoV-2 increases the risk of thromboembolic complications and patients in the ICU are mostly lying in beds – prevention is necessary for all patients!
- Vibrating chest massage – a device inducing vibrations of the chest facilitates detachment of airway secretions in the lungs and stimulates its relocation to the upper respiratory tract, where it can be evacuated.
- Chest tapping – facilitates evacuation of airway secretions.
- Positioning patients on their stomach – very important, according to some research this position promotes regeneration of lungs both in patients who are mechanically ventilated and those who breathe spontaneously. A physiotherapist’s role involves placing the patient in the right position and correcting his/her posture while he or she lies on the stomach, in order to prevent complications.
- Passive exercises – maintenance of mobility in joints – from the very beginning of a patient’s stay in the ICU.
- Passive-active exercises for patients in analgosedation or conscious.
- Active exercises – for conscious patients.
- Education on using the TriFlow device – practicing breathing with resistance on inhalation and exhalation.
- Verticalization.
- Mobilization.
- Discharge to another ward – wonderful moment awaited by the patient, for which we all work very hard. Discharge summary should include description of implemented physiotherapy, current condition of a patient and future recommendations.
Let’s support our patients
It needs to be emphasized that when a patient is conscious and verbally responsive, he or she requires a lot more time and attention. Since these patients usually spend several weeks in hospital, they have no contact with their family and friends due to sanitary restrictions. As a patient slowly recovers, it is very important to ensure psychological support and allow the patient to talk to a therapist or other healthcare professionals. In this challenging and often difficult to understand situation (for both us and the patients) let’s show our patients as much interest and kindness as possible.
When we share our experiences with family and friends, they call us heroes – as people tend to call everyone in the front line. We really don’t feel like heroes. But we do hope that if we ever face a similar challenge in the future, we will deal with it as good as we’re doing it now, or even better.